
"Hope matters”: Tobechukwu’s story
March 26, 2026
Tobechukwu was diagnosed with congenital diaphragmatic hernia (CDH) during a routine scan which meant the beginning of a long journey filled with surgeries, setbacks, and intensive care. During this journey, Ronald McDonald House Tooting became a lifeline for his parents for 342 nights, offering comfort and practical support during the hardest times.
Despite many delays and emotional challenges, Tobechukwu gradually improved and was finally discharged. Now, after ten months at home, he is thriving, off oxygen, and feeding orally, which is the miracle his parents prayed for throughout his hospital stay.
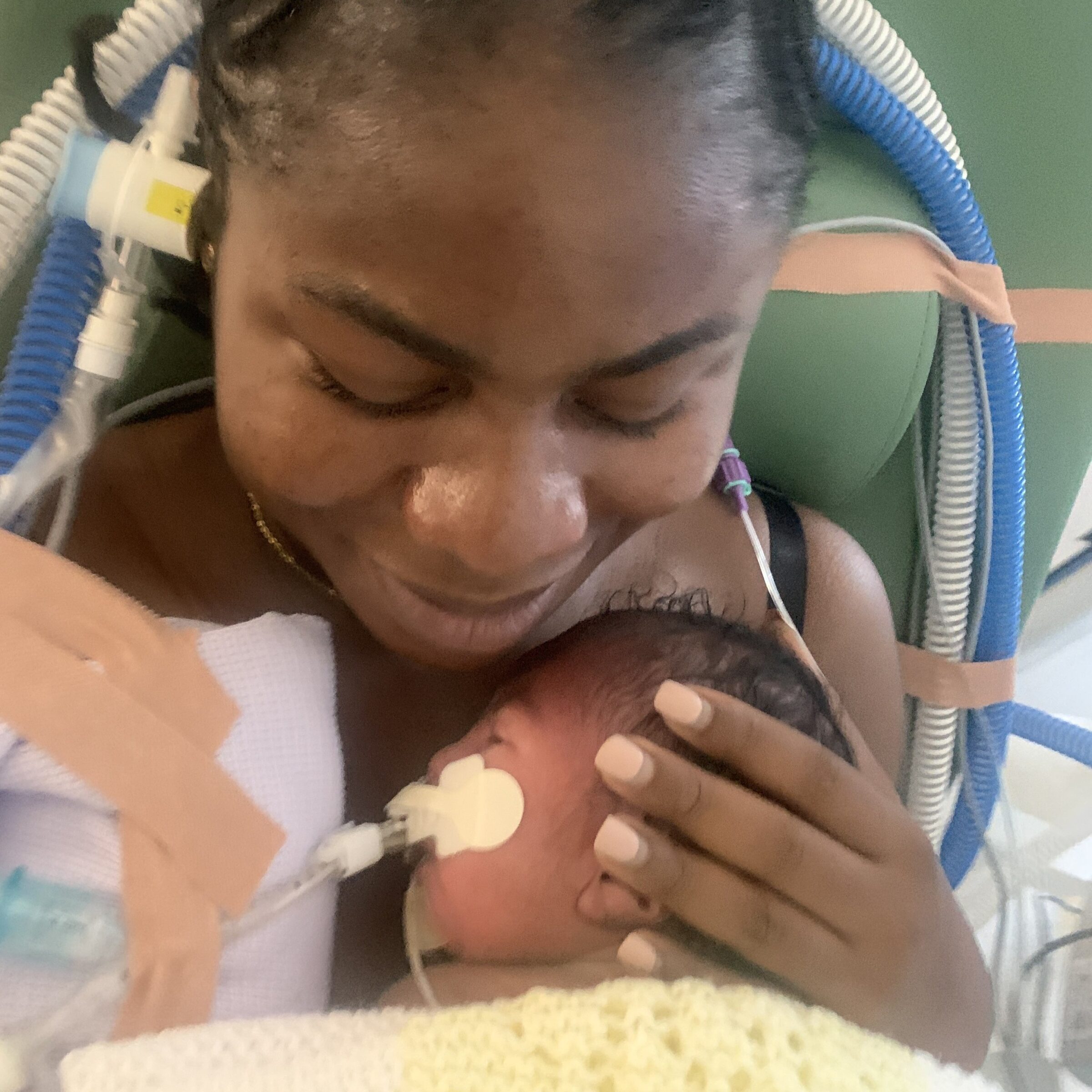
Guest blogger: Omobolanle
We attended a routine scan when I was 23-weeks pregnant. It was during this appointment that we learned our baby had been diagnosed with congenital diaphragmatic hernia (CDH).
CDH occurs when the diaphragm doesn’t form properly, leaving a gap between the chest and the abdomen. I initially thought that being in my second trimester, there was still time for things to develop, but the doctors explained that the diaphragm should have closed during the first trimester. We were in shock. They told us we would be referred to St George’s Hospital to see a specialist and just two days later, we met with the consultant who confirmed the diagnosis. That was the beginning of our journey.
We were given leaflets with more information and were told that there was a 50/50 chance of survival if we chose to continue with the pregnancy . We had so many questions about what it would be like to manage a child with CDH in the long term and were reassured that it could be managed with regular hospital visits and ongoing care.
We were also referred to King’s College Hospital for further testing to confirm the diagnosis. It was there that we learned about a procedure called FETO (Fetoscopic Endoluminal Tracheal Occlusion). This involved performing surgery while I was still pregnant, where a balloon would be inserted into our baby’s trachea. Due to the CDH, Tobechukwu’s organs had shifted into his chest, compressing one of his lungs and preventing it from developing properly, meaning that only one of them was growing. The surgery aimed to move the organs away from the chest to create space for the lungs to develop, significantly increasing his chances of survival after birth.
Because of the complexity of his condition, the doctors advised against delivering him at our local hospital. After the procedure, we began attending weekly check-ups at King’s College Hospital to closely monitor his progress. The FETO surgery was performed at 27 weeks, and it involved putting Tobechukwu to sleep while still in the womb. The balloon remained in place until 33 weeks and during that time, we were told that if anything went wrong, he wouldn’t be able to survive it. Once we passed that critical stage, the doctors scheduled a controlled delivery. They wanted to avoid the risks associated with going past 40 weeks, as the placenta might not have remained effective. Tobechukwu was born at 38 weeks and 4 days at St George’s Hospital, where a specialist team was ready to support him.
On the morning of Tobechukwu’s birth, the medical team broke my waters and connected a monitor directly to his head while he was still in the womb to track him. He was born on the 23 May 2024, around 3pm. The room was filled with specialists, all prepared to take immediate action. I was able to hold him for just a few seconds before he was taken away to be intubated. Ten days later, they performed a surgical procedure known as the Ladd’s procedure to reposition his organs, moving them from the chest back into the abdominal cavity and to close the gap in his diaphragm. His body was extremely swollen following the surgery, and for days he remained very still, mostly sleeping and recovering.
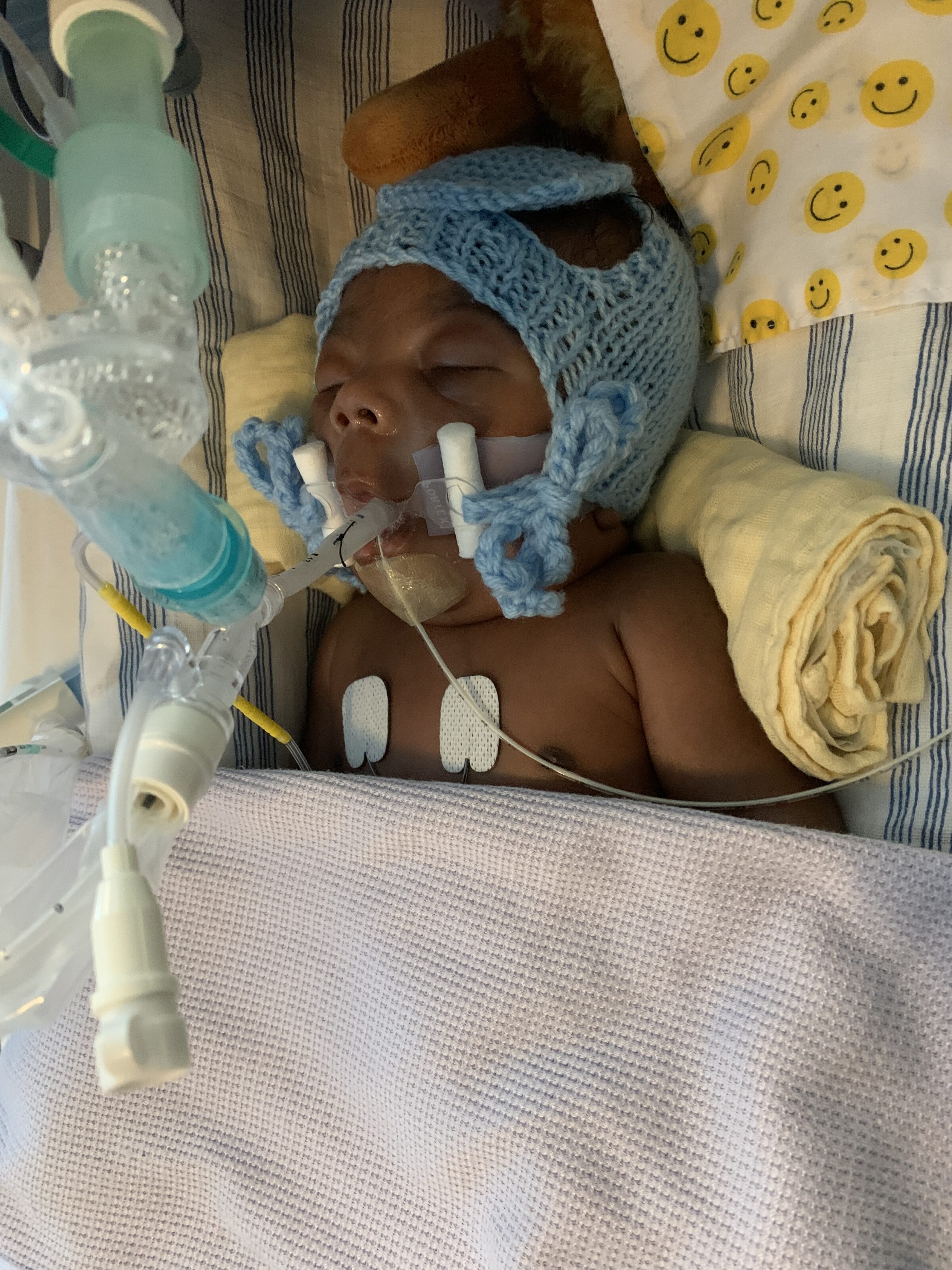
By July, Tobechukwu was finally off the ventilator, and we felt hopeful. He was receiving regular oxygen support, and things seemed to be improving. Like many babies with CDH, he experienced reflux, so he was given an NG tube to help deliver his milk directly to his stomach. Not long after, he was moved from the Intensive Care Unit (ICU) to the High Dependency Unit (HDU), which felt like a step forward. But soon, his oxygen saturation levels began to drop. After just a week on HDU, we received a call saying he wasn’t doing well. By the time I arrived, he was already being moved back to ICU and intubated again.
I was absolutely devastated. I had so many questions and fears. This setback meant starting treatment all over again. His condition fluctuated and he battled infections, severe reflux, and other complications. Because of the persistent reflux, he was fitted with an NJ tube, which bypasses the stomach and delivers nutrition directly to the intestines. He remained in ICU from July through October. That’s when the doctors told us we’d be in hospital much longer than we had originally expected. We had to learn how to manage his tubes ourselves, especially over weekends when consultants weren’t available. During our time in the Neonatal Unit, we spoke with other families about their experiences. We were surprised to hear that many had been there for a few months and at the time, we had no idea our journey would be so much longer.
By the end of the year, he began showing signs of improvement, and we started having conversations about possibly transferring to our local hospital. But once again, things took a turn. His condition became unstable, and the transfer had to be put on hold. As he grew, he could no longer be cared for in the neonatal unit, so we were moved to the Paediatric Intensive Care Unit (PICU). That meant we would be spending Christmas in the hospital.

Our journey began again on PICU, and everything felt different, more intense and more frightening than what we had been used to. This time, he needed a ventilating mask over his face, which he found very uncomfortable. He cried often and seemed constantly unsettled. As his condition improved, he was moved to the Paediatric Step-Down Unit (PSDU), where we began learning how to care for him at home. The dynamic shifted and now it was the nurses observing us, rather than us watching them. We had to take on more responsibility, learning how to manage his care independently.
We were given the opportunity to do an overnight stay at home to see how we would cope which went really well. We started doing more home visits, and everything was pointing towards discharge. But just as we were preparing to leave, Tobechukwu caught rhinovirus and developed sepsis again. That meant another week in hospital.
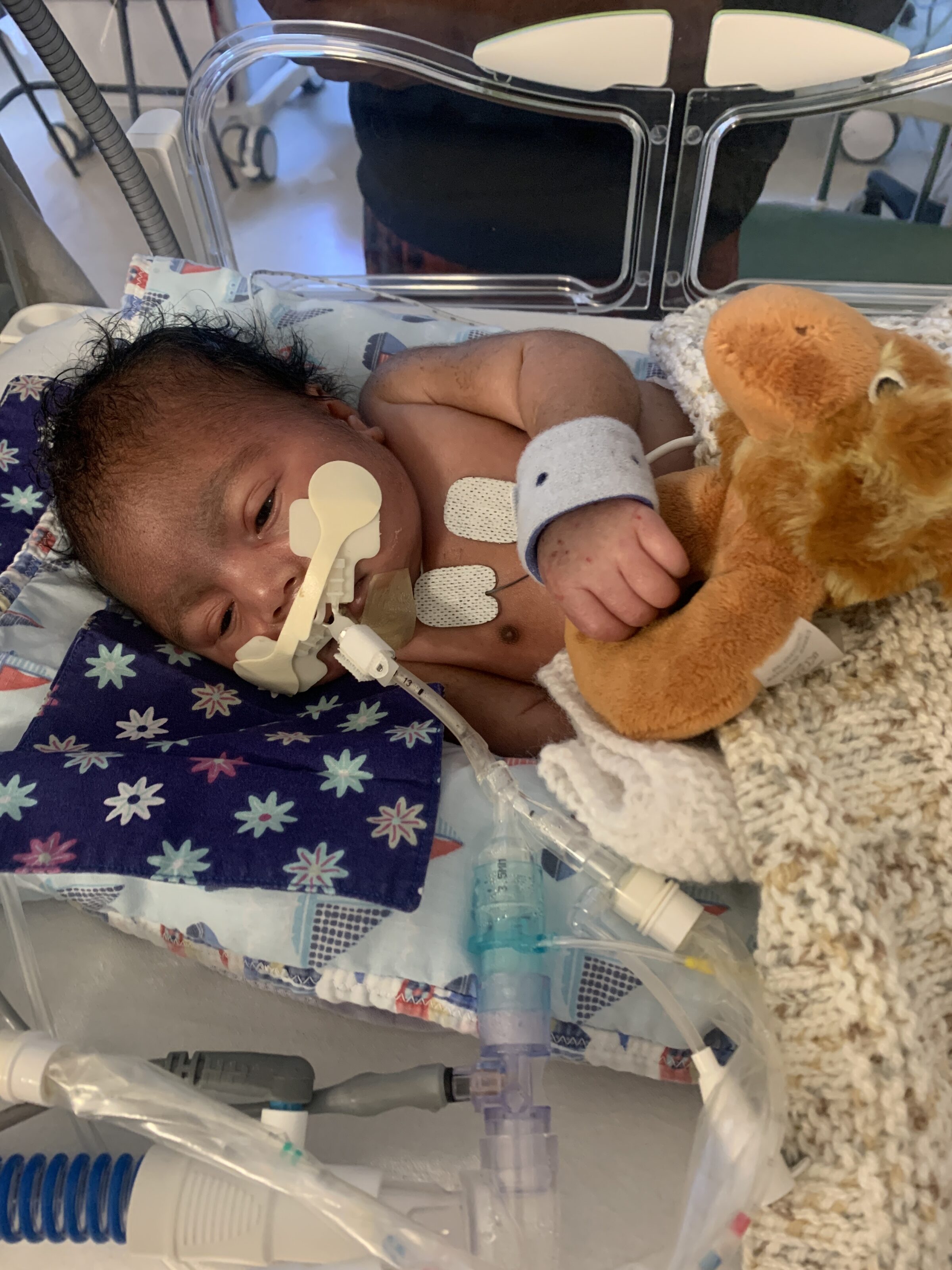
We first learned about Ronald McDonald House from our family care nurse and from the moment we arrived, it felt like a ‘home away from home’- calm, comforting, and safe. It helped ease the ache of missing our actual home. We could sleep well, cook meals, and live with a sense of normality. Everything we needed was there. The staff were incredible, always smiling, checking in, and offering reassurance. Their warmth made a huge difference. I especially looked forward to Mondays when the food deliveries arrived, it was a small joy that lifted my spirits.
We made so many friends at the House. At the beginning of this journey, we felt isolated, but being surrounded by other families going through similar experiences helped us feel less alone. The Tooting House was a lifeline and being close to the hospital meant we could respond quickly to emergencies without the exhausting commute from Crawley. Without it, we would’ve had to rent a place, constantly worrying about costs and moving around. The House gave us the stability we needed to be the best version of ourselves for our baby. Seeing other families leave gave us hope that our day would come too, even if our journey was longer than expected.
Leaving the House was emotional, it felt like moving out of a home where we had lived and grown but taking him home as a family for the first time was a beautiful moment. We’ll miss the staff and the families we met, but we left knowing we’ve formed lifelong friendships. The House is forever part of our story.

We’ve now been home for ten months, and our baby has come such a long way. He is almost two-years old, no longer on oxygen, and the NJ tube is gone. He’s thriving, starting to feed orally, making sounds, and showing us his happy personality every day.
If you’ve read our story, you’ll understand just how vital this House is. Every donation goes to a truly meaningful cause. We’re so grateful for how far we’ve come, it almost doesn’t feel real that we spent nearly a year in hospital. CDH affects one in 5,000 babies, and to any family facing this or anything else: never lose hope. We were given the option to let go, but we held onto faith. Our baby is living proof that hope matters.

Help us provide free home away from home accommodation to support families with children in hospital with a donation.

