Maternal Mental Health: A Thought-Leadership Piece
September 16, 2019
Having a baby is a huge life-changing event creating lots of emotional and physical strains. It is natural for women to experience a range of emotions during and after pregnancy. But for some, it can be more than just ‘baby blues’ or tiredness. They could, in fact, be experiencing a maternal mental health issue.
Perinatal mental health problems can occur during pregnancy or in the first year following the birth of a child. Around 1 in 5 women experience some type of perinatal mood and anxiety disorder (PMAD). PMADs cover a wide range of conditions including depression, anxiety, obsessive-compulsive disorder, psychosis and PTSD (post-traumatic stress disorder). If left untreated, PMAD can have significant and long-lasting effects that impact not just the mum but her whole family.
The PANDAS Foundation is a UK-wide perinatal mental health charity which offers peer-to-peer support and signposting for parents struggling. Annie Belasco, Head of PR and Fundraising at PANDAS, said,
“Baby Blues is a common term used, which can be a dangerous assumption of low mood. And experiences such as isolation and loneliness are also factors that can contribute to mental illness. We are here to support service users by focusing on self-care and next steps. We recruit regularly to meet the needs of the growing numbers of parents who are concerned about their perinatal mental health. Supporting a stretched and under-resourced NHS, who are unable to meet the needs of every parent that does not appear to be at ‘crisis level’ or parents that cannot access the support they need.”
FAMILIES WITH BABIES IN THE NEONATAL UNIT NEED LOTS OF SUPPORT
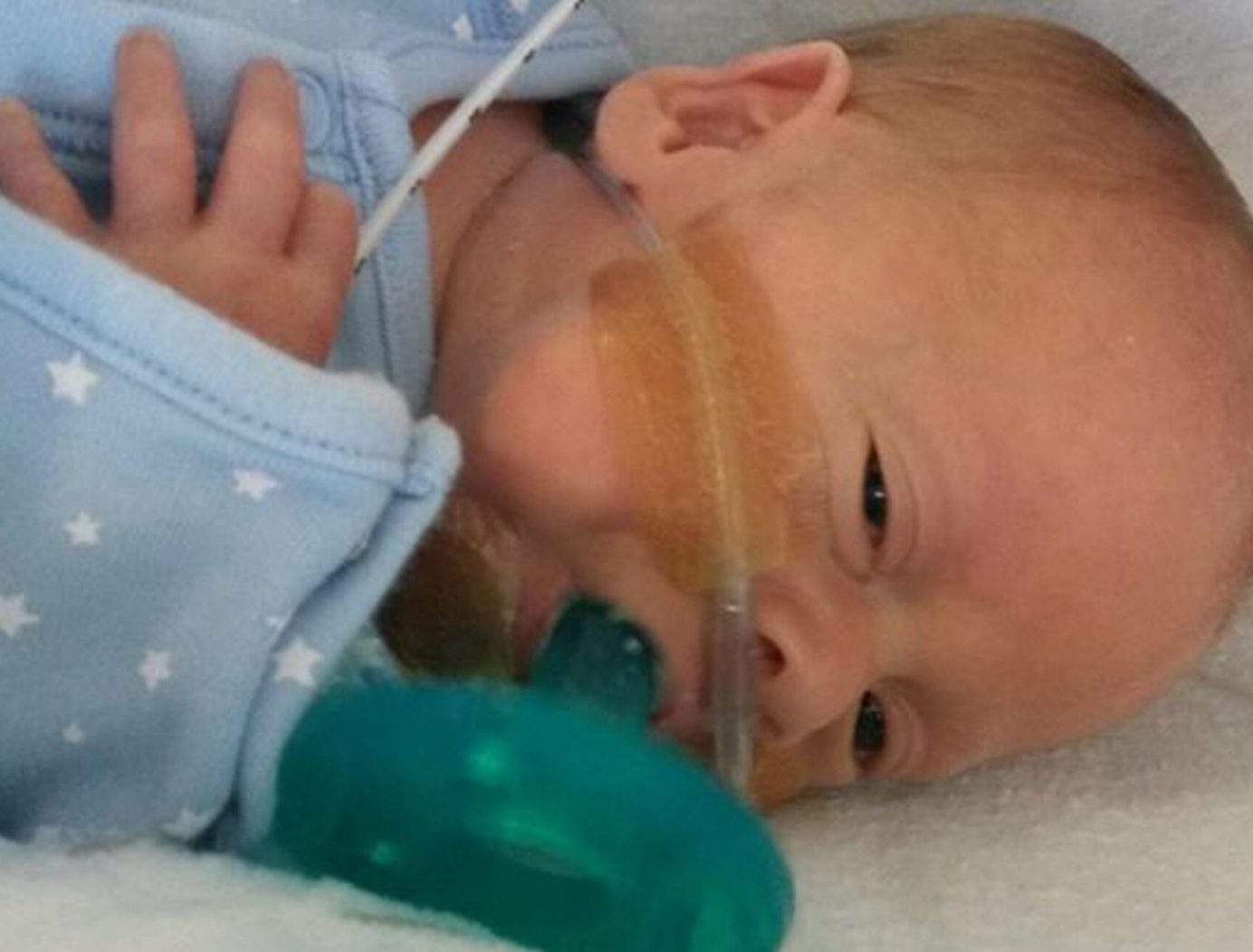
Having a baby can be a very exciting time, but when your baby is born prematurely, the anticipation of a new arrival is dramatically interrupted. Some women suffer a traumatic birth, or their baby is very ill with a medical condition they were unaware of during pregnancy. All families affected find themselves shocked and fearful in the neonatal intensive care unit (NICU).
FIONA LAWSON is an experienced Neonatal Services Matron based at Southampton Children’s Hospital. She is all too aware of the challenges faced by parents of very sick babies in NICU.
“It’s important to acknowledge how having a premature baby or a very sick baby at birth isn’t what anyone hopes for. When you first get pregnant you automatically imagine your future with a healthy child and what’s happened has actually ruined all those plans. There’s a cycle of grief for the parents of a premature baby. Some families sail through it and for others it’s awful and it’s not unusual for neonatal families to have post-traumatic stress disorder (PTSD), it can be very significant.”
IT IS ESTIMATED THAT ABOUT 40% OF NICU MUMS SUFFER FROM POSTNATAL DEPRESSION COMPARED WITH 5-10% OF MOTHERS WHO GIVE BIRTH TO FULL-TERM HEALTHY BABIES.
Having a premature, birth-injured or sick baby can lead to extreme anxiety. The NICU is an intense unnatural environment full of machines that beep, with lines and wires, where the parents sit powerless watching their babies fight for their lives. It is estimated that about 40% of NICU mums suffer from postnatal depression compared with 5-10% of mothers who give birth to full-term healthy babies. Of that number, more than 50% report symptoms of anxiety and PTSD. These are stark statistics and like many aspects of mental health, it is not talked about openly enough.
Sam stayed at Ronald McDonald House Arrowe Park in Merseyside after she gave birth to twins 14 weeks premature. Sam spoke to us about her struggle with postnatal depression and PTSD.
“It’s really hard to explain the journey you go through with premature babies. Nothing can physically, mentally or emotionally prepare you for it. Even if someone was to sit you down and tell you all about it – you still wouldn’t be prepared.
“I’ll never forget seeing my babies for the first time, covered in wires from head to toe and connected to a machine that was keeping them breathing. As a mother, you’re meant to protect your child through everything, but in NICU there’s nothing you can do.
“I was emotional. If you told me good news – I’d cry; if you told me bad news – I’d cry, and if you told me no news at all – I’d still cry.
“I became aware of my postpartum depression when my son, who was most unwell, started to get better. I thought it was all in my head and I was just overwhelmed by it all, but it was more than that.
“Even to this day 16 months on, I can still hear the noises the machines made in the NICU. I can still see like it was yesterday, the nurses rushing to my baby’s side because he had stopped breathing.”
There is a huge amount of uncertainty in the NICU. Some babies get transferred quickly, while others spend the first year of their lives there. The specialist care required is usually unavailable at a local hospital, so the families find themselves far away from home. This is where Ronald McDonald House Charities UK provides invaluable support by offering free family-friendly accommodation so they can stay together close to their sick child in hospital.
This is vital for the baby in the NICU, but it also supports the emotional wellbeing of the parents. Fiona Lawson knows this better than most.
“To help them with the psychological impact of having a very sick baby, the longer they spend with their baby and be involved with its care, the better the outcome is for the whole family.
“Having a Ronald McDonald House means that families can stay at the hospital, spend more time in the unit and be close to their baby. The NICU is a fast-paced and hectic environment and sometimes babies just need to be touched and held, and that’s extremely difficult for us to fulfil and it’s also not our job, that’s the role of the parent. We work hard with the family to facilitate what we call ‘kangaroo care’ or ‘skin-to-skin’ contact between baby and parent, and it’s known to have an amazing psychological effect on the parents and a positive physiological impact on the baby.”
NATOMIE REID-LYON is an Early Help Lead in the safeguarding team at Birmingham Women’s and Children’s Hospital. Her work includes working across paediatrics inpatient at Birmingham Children’s Hospital site and neonatal intensive care unit at Birmingham Women’s Hospital.
“Parents can feel powerless and isolated in the NICU and become unsure of their actual role. Their baby is being cared for by the nurses and other health professionals and they feel like a bystander on the periphery unsure and unable to interact with their own child. Being present and involved in the care of the child is so important.
“The parents also need to understand the medical condition and often it’s a lifelong condition which they need to manage and live independently with in the community once discharged home.”
Identifying parents who are struggling with their mental health can be difficult within hospital environment and Natomie focuses on raising awareness, reducing the stigma of PMAD and supporting staff to be more mindful of the potential signs and symptoms.
“In the NICU, everyone’s focus is on the baby and getting that baby well. Some parents don’t want to admit they can’t cope as though there’s a stigma attached to it. The medical staff are working to save their baby’s life and they don’t want to take that attention away. Parents prioritise their baby over their own health and wellbeing and put how they’re feeling inside on hold and mask their physical signs.
“We have a programme of reminding and training staff here to bring PMAD to the forefront, so staff are more mindful of the signals to help identify those parents who are, for example, not interacting with their child.
“It’s also important to communicate with Ronald McDonald House and be alerted to parents who leave the NICU at the end of the day and then let their guard down and show serious signs of not being able to cope.
“We have had parents not present in the NICU as much as we would like, and it’s been because they’ve been feeling too low to leave their room. Help is always available, and we want to ensure all parents get the support they need.”
PMAD CAN AFFECT THE WHOLE FAMILY
Often when families are discharged from hospital and return home, they suddenly realise what they have gone through during the past weeks or months. Making that transition from hospital to home, often with a child still requiring medical treatment, is daunting and that is sometimes when PMADs become apparent.
Research estimates 7 in 10 mums hide or downplay their PMAD symptoms. It is important there is support from health visitors and GPs. Without understanding, advice, and treatment these mental illnesses have a devastating impact on the women affected and on their partners and families.
Many people do not realise that about 1 in 10 dads develop depression during this time. If there are other children, they too are affected, and their daily routine of nursery or school is interrupted. An integrated approach to family mental health allows both parents to move beyond the postpartum period as a thriving family unit.
GRIEF IS A PERSONAL JOURNEY
Sadly, the death of a baby soon after birth is not a rare event; over 2,000 babies die every year in the UK within the first four weeks of life. The loss can happen suddenly or following a prolonged battle for survival in the NICU. It is estimated that 20-25% of pregnancies end in miscarriage or stillbirth. Grief will affect the whole family and it is not unusual for mums and dads to also experience postpartum depression.
PATRICIA MCGURK is a bereavement counsellor at St George’s Hospital, which has a Ronald McDonald House for families, and she explained how the loss of a baby affects people’s mental health in different ways.
“The death of a baby is devastating for all of the family; and it’s important to realise that it affects mums, dads/partners and siblings. It’s exciting waiting for your baby to be born and you make plans and imagine your life together. The arrival of a premature baby or very sick full-term baby usually comes hand-in-hand with a traumatic birth, and that compounds the impact of loss.
“Bereavement can be overwhelming and feel like it’s taking over everything. It manifests itself physically and emotionally; and the intensity of feelings can be frightening. Physical symptoms may be chest pains, shaking, heart palpitations and sickness. It’s normal to not have an appetite but important to keep eating and drinking to remain physically strong to cope with the emotional trauma. It’s not uncommon to find it difficult to sleep and to experience dreams and nightmares. This can lead to exhaustion and feeling run-down physically and emotionally.”
Many symptoms of grief are like symptoms of postnatal depression, it can be difficult to tell them apart. People might also show signs of post-traumatic stress disorder (PTSD). It is important that they seek professional advice from a GP or health visitor or ask family and friends to get help.
RONALD MCDONALD HOUSE IS INVALUABLE
Ronald McDonald House Charities UK provides free accommodation for families with a sick child in hospital, so they can live close-by in an understanding environment during a very difficult part of their life. Often families have to travel many miles to access the specialist medical care their child needs. The financial impact of accommodation and travel expenses can be huge alongside having a mortgage, bills and possibly not being able to work while your child is unwell far away from home.
Natomie at Birmingham Children’s Hospital has seen the financial impact on families and how it affects their emotional wellbeing.
“We have families who were already struggling financially before their baby arrived so to be faced with accommodation and travel costs to and from the hospital is a big burden that they’ve not been able to budget for.
“Being able to stay at the Ronald McDonald House reduces the travelling involved which helps emotionally and physically.”
Everyone in Ronald McDonald House understands the rollercoaster medical journey that parents are on. Staff in the Ronald McDonald Houses are always on hand to listen and provide support; sometimes that is ensuring they get help from the hospital, advice online or in their local community. Sometimes, the most valuable support can come from a support network of other parents staying at the House, who are experiencing the same trauma. Fiona summed this up perfectly when she said,
“Families staying at Ronald McDonald House meet other neonatal families and also families who’ve come through NICU with their baby now receiving specialist paediatric care, and it helps them understand and process what they’re going through. Peer-to-peer support is a real help during this difficult time and it’s something we encourage; it helps parents when they see others like them touching their ventilated babies, tube feeding and changing their bed.”
WHERE TO GET HELP
If you’ve been affected by this article and need to talk to someone about mental health issues, please find below some organisations which can support you.
PANDAS is a UK-wide perinatal mental health charity which offers peer-to-peer support and signposting for parents struggling. Visit their website for information about their telephone support line.
The Mind Infoline provides information on a range of topics including types of mental health problems and where to get help. They will look for details of help and support in your own area. Tel: 0300 123 3393 – Email: [email protected] – Text: 86463.
Alternatively, you can contact your GP for support. Visit the NHS website for advice about post-natal depression, information about the symptoms of post-natal depression, and how your local GP can help.
Help us provide free home away from home accommodation to support families with children in hospital with a donation.

